위장관 기질종양: TNM병기와 National Institutes of Health 분류에 대한 예후 비교 분석
ABSTRACT
Purpose
The main limitation of the National Institutes of Health (NIH) consensus criteria is the biological and prognostic heterogeneity of tumors while the utility of the newly proposed UICC TNM staging system has not yet been validated. Our object is to compare the overall and disease-free survival (DFS) of patients with gastric gastrointestinal stromal tumors (GIST) using the UICC TNM staging system and the NIH consensus criteria and to determine the optimal risk stratification system for GIST.
Methods
Retrospective analysis of 164 patients who underwent operative management for primary gastric GIST between 1994 and 2004.
Results
The overall five-year survival rate was 89.6%. In the 149 patients who underwent an R0 resection, the five-year DFS rate was 86.3%. According to the NIH consensus criteria, the five-year survival rate after resection was 100% for patients in the very low-, low-, and intermediate-risk groups and 71.9% for patients in the high-risk group. The UICC TNM stages IA, IB, and II had the same survival rates (100%) and stage IIIA (75.0%) and stage IIIB (69.5%) showed no significant difference in survival compared to the NIH criteria, which precluded better risk stratification. The patients who were included in the high-risk group by NIH consensus criteria (>10 cm, ≤5/50 high power field) and were stage II by the UICC TNM staging system had a 100% five-year survival rate.
Conclusion
Using the current schemes, one system does not demonstrate superior prognostic ability over the other. However, the high-risk group (T4/low mitotic rate) and stage II patients appear to be appropriately classified.
Keywords: Gastrointestinal stromal tumors, Neoplasm staging, Classification
INTRODUCTION
Gastrointestinal stromal tumors (GIST) are rare mesenchymal tumors arising from the gastrointestinal tract and are the most common non-epithelial sarcoma, according for 0.1%–3% of all gastrointestinal malignancies. The most common anatomical site of origin is the stomach (60%–70%), followed by small intestine (20%–30%), esophagus (less than 10%), and colorectum (5%) [ 1– 3]. Before risk stratification of GIST had been established, the French Federation of Cancer Centers grading system for sarcomas was used, but many reports showed the system did not accurately reflect the clinical manifestations of GIST [ 4]. In 1993, Amin et al. introduced clinicopathologic criteria for assessing the malignant potential of GIST by examining factors such as peripheral invasive growth, lymph node metastasis, distant organ metastasis, peritoneal dissemination, and recurrence to allow classification of GIST as benign, borderline, or malignant according to tumor size and mitotic rate [ 5]. The National Institutes of Health Consensus risk score (NIH consensus criteria) was introduced in 2001 and categorized tumors into four risk groups based on tumor size and mitotic rate: very low-risk, low-risk, intermediate-risk, and high-risk [ 1]. One of the tenets of this risk stratification schema is that virtually all GISTs (especially those larger than 1 cm) have malignant potential, a concept supported by three large retrospective studies from the Armed Forces Institute of Pathology (AFIP) [ 2, 6, 7]. The AFIP series represent the largest published experience with GISTs diagnosed and treated in the modern era for which long-term clinical follow-up is available [ 8]. They also served to validate and expand the 2002 consensus criteria, confirming the results of earlier studies indicating that anatomic location affects the risk of disease recurrence [ 9]. In general, intestinal GISTs are more aggressive than are gastric tumors. The differences in outcome between gastric and small bowel GISTs can be illustrated by the published experience of AFIP [ 6, 7]. Taken together, these studies indicate that all GISTs larger than 2 cm have some finite risk of recurrence, while gastric GISTs that are 2 cm or less in size with a low mitotic rate can be regarded as having an exceedingly low recurrence risk. However, until long-term data on the natural history of GISTs <2 cm in size from all sites are known, it is misleading to regard any as being truly benign. Huang et al. published the modified NIH consensus criteria, combining the very low- and low-risk groups into risk level I, classifying the intermediate-risk group as risk level II, and dividing the high-risk group into risk level III and IV [ 10]. However, this modification does not take disease site into account. The importance of small bowel location as an indicator of poorer long-term outcomes was confirmed in an analysis of data from the phase III adjuvant imatinib trial, ACOSOG Z9001 [ 11]. Largely based upon data from the AFIP series [ 6, 7], the seventh edition of the UICC TNM system (UICC TNM stage) was released [ 12]. It presented the lymph node stage and metastasis for the first time. The principle aim of the UICC TNM stage was to facilitate a uniform and standardized analysis of malignant tumors based on their stage. The aim of this study was to validate and compare the performance of the NIH consensus criteria and the UICC TNM stage in a primary gastric GIST resected at a single institution to determine the ideal risk stratification scheme. In this study, we performed comparative analysis on the disease-free survival (DFS) and overall survival using the UICC TNM stage and the NIH consensus criteria and assessed the benefit of the sub-classification of tumors in the high-risk category.
METHODS
From 1994 until 2004, 8,321 patients underwent gastrectomy under any diagnosis at Samsung Medical Center, Sungkyunkwan University School of Medicine (Seoul, Korea). One hundred and sixty four patients who underwent resection for a primary gastric GIST were enrolled. Retrospective analysis of clinical, pathologic, and radiologic data, and follow-up information was performed on the basis of medical records. The tumor size was defined with the largest diameter recorded at pathologic report. Risk scores were stated based on the clinicopathologic characteristics and classified according to each set of criteria to allow for comparisons. The exclusion criteria were (1) synchronous malignancies and (2) inaccurate medical records. The Institutional Review Board at Samsung Medical Center approved this study.
Pathology
Pathologic diagnoses of gastric GIST were confirmed by hematoxylin-eosin staining (H&E staining). An expert gastrointestinal pathologist reviewed all of the cases, and one case of schwannoma and two leiomyomas were excluded from this study. Additional immunohistochemical staining (c-kit) was performed in 113 (68.9%) cases to confirm the pathologic diagnosis and medical treatment. Approximately 95% of GISTs have positive results [ 13]. Nevertheless, the most important diagnostic tool for GIST remains the hematoxylin and eosin-stained section [ 14].
Surgical treatment
R0 resection was defined as complete resection of the localized tumors. Gross and pathologic R1 resection was defined as resection of all clinically evident disease. R1 resection included tumors extending to a resection margin, or tumors with a very thin capsule dissected away from other organs, or cases with tumor rupture before or during operation. R2 resection was defined as the presence of a macroscopic residual tumor. Wedge resection was performed if the margin could be secured regardless of the location of the lesion. Subtotal or total gastrectomy was performed if margins could not be secured. Imatinib mesylate was administered to 30 patients who had distant metastasis at the time of exploration, or incomplete resection, or recurrence after R0 resection.
Tumor classifications
NIH consensus criteria and UICC TNM stage were demonstrated in Table 1. Very low-risk and low-risk groups per the NIH consensus criteria were included in stage IA. In the intermediate risk group, patients with tumors measuring 5–10 cm in size and a mitotic count ≤5/50 high power field (HPF) were classified as stage IB, while patients with tumors ≤5 cm and a mitotic count of 6–10/50 HPF were classified as stage II. In the high-risk group, patients with tumors ≤10 cm and a mitotic count ≤5/50 HPF were classified as stage II. Patients with tumors measuring 5–10 cm and a mitotic count >5/50 HPF were classified as stage IIIA, and patients with tumors >10 cm and a mitotic count >5/50 HPF were classified as stage IIIB. Patients with lymph node metastasis or distant metastasis or tumor rupture during surgery were classified as stage IV.
Table 1.
Comparison of patient distribution for NIH consensus criteria and the UICC TNM staging system
NIH consensus criteria
|
UICC TNM staging system
|
|
Tumor size (cm) |
Mitotic rate (/50 HPF)
|
T stage (tumor size, cm) |
Mitotic rate (/50 HPF)
|
|
≤ 5 |
6–10 |
> 10 |
≤ 5 |
5 > |
Any rate |
|
≤ 2 |
Very low: 5 (3.0) |
Intermediate: 1 (0.6) |
High: 2 (1.2) |
1 (≤ 2) |
IA: 5 (3.0) |
II: 3 (1.8) |
|
|
2–5 |
Low: 66 (40.2) |
Intermediate: 8 (4.9) |
High: 6 (3.7) |
2 (2–5) |
IA: 66 (40.2) |
II: 14 (8.6) |
IV |
|
5–10 |
Intermediate: 29 (17.7) |
High: 4 (2.4) |
High: 13 (7.9) |
3 (5–10) |
IB: 29 (17.7) |
IIIA: 12 (7.3) |
(N1 or M1): 18 (10.9) |
|
> 10 |
High: 5 (3.0) |
High: 6 (3.7) |
High: 19 (11.7) |
4 (> 10) |
II: 2 (1.2) |
IIIB: 15 (9.2) |
|
Statistical analysis
The Kaplan-Meier method was used for survival analysis and the survival difference was analyzed using the log-rank test. Multivariate analysis was performed using Cox's proportional hazards model. Statistical analysis was conducted using PASW ver. 17.0 (SPSS Inc., Chicago, IL, USA). A P-value <0.05 was considered statistically significant.
RESULTS
Patient characteristics
Of the 164 patients, 86 were males and 78 were females. The median age was 57 years (range, 16–79 years). The median tumor size was 5.6 cm (range, 1.5–26 cm) and the median mitotic rate was 4 (0–340) per 50 HPF ( Table 2).
Table 2.
Patient clinicopathologic characteristics
|
Characteristic |
Median (range) |
No. (%) |
|
Age (yr) |
57 (16–79) |
|
|
Sex |
- |
|
|
Male |
|
86 (52.4) |
|
Female |
|
78 (47.6) |
|
Tumor size (cm) |
|
≤ 2 |
1.8 (1.5–2.0) |
8 (4.9) |
|
> 2 and ≤ 5 |
3.8 (2.2–5.0) |
80 (48.8) |
|
> 5 and ≤ 10 |
6.5 (5.3–10.0) |
46 (28.1) |
|
> 10 |
15 (10.5–26) |
30 (18.2) |
|
Mitotic rate (/50 HPF) |
|
≤ 5 |
2 (0–5) |
105 (64.0) |
|
> 5 and ≤ 10 |
7 (6–10) |
19 (12.0) |
|
> 10 |
27 (11–340) |
40 (24.0) |
|
Type of operation |
- |
|
|
Wedge resection |
|
114 (69.5) |
|
Subtotal gastrectomy |
|
24 (14.6) |
|
Total gastrectomy |
|
24 (14.6) |
|
Exploratory laparotomy |
|
2 (1.3) |
|
Resectability |
- |
|
|
R0 |
|
149 (91.0) |
|
R1 |
|
6 (4.0) |
|
R2 |
|
9 (5.0) |
|
NIH consensus criteria |
- |
|
|
Very low |
|
5 (3.0) |
|
Low |
|
66 (40.2) |
|
Intermediate |
|
38 (23.2) |
|
High |
|
55 (33.6) |
|
UICC TNM stage |
- |
|
|
IA |
|
71 (43.2) |
|
IB |
|
29 (17.7) |
|
II |
|
19 (11.6) |
|
IIIA |
|
12 (7.3) |
|
IIIB |
|
15 (9.2) |
|
IV |
|
18 (10.9) |
Patient distribution
Our patients were classified into four groups according to the NIH consensus criteria and six groups according to UICC TNM stage ( Table 1). According to UICC TNM stage, 5 patients who were included in the very low-risk group and 66 patients in the low-risk group were all classified as stage IA. Twenty nine of thirty eight patients in the intermediate-risk group were classified as stage IB, and the remaining 9 patients were classified as stage II. Fifty five patients in the high-risk groups were divided into four stages: stage II (10 patients), stage IIIA (12 patients), stage IIIB (15 patients), and stage IV (18 patients).
Surgical management
Wedge resection was performed in 114 patients, including 2 patients undergoing laparoscopic wedge resection. Subtotal and total gastrectomy was performed in 24 patients and 24 patients, respectively. Exploratory laparotomy without resection was performed in 2 patients because of tumor dissemination. One patient had omental seeding with liver metastasis, and the other had seeding in the peritoneum with the rectal shelf. R0 resection was performed in 149 patients and R1 resection was performed in 6 patients. The mass ruptured intraoperatively in 5 of these 6 patients, and the other patient, who underwent resection of seeding nodules and the invaded organs, had microscopic residual tumors in the invaded organs. Among 9 patients with R2 resection, four had peritoneal seeding, three had peritoneal seeding with rectal shelf metastasis, and one had peritoneal seeding with liver metastasis. The other one had only liver metastasis in both lobes.
One hundred and nine patients who were included in the very low-, low-, and intermediate-risk groups according to the NIH consensus criteria underwent R0 resection. In the high-risk group (n=55), 40 patients underwent R0 resection and 6 patients underwent R1 resection, and 9 patients done R2 resection. According to UICC TNM stage, R0 resection was performed for all stage IA, IB, II, and IIIA patients (n=135). 14 patients of 15 stage IIIB patients underwent R0 resection, and 1 patient underwent R1 resection. Among the patients of stage IV (n=18), 4 patients underwent R0 resection, 5 patients underwent R1 resection, and 9 patients underwent R2 resection.
Immunohistochemical staining
Immunohistochemical staining was performed in 139 of 164 patients (84.6%). C-kit expression was tested into 113 cases (68.9%), and positive c-kit was found in 110 cases (97.3%). CD34 was positive in 93/100 (93%), smooth muscle actin in 53/108 (49%), S-100 in 18/109 (17%), and Ki-67 in 14/75 (19%) cases of tumors, respectively. Ki-67 staining was defined as positive when the stain was greater than 10% of tumor dimension.
Recurrence
Recurrences were found in 19 patients of whom underwent an R0 resection (n=149) ( Table 3). These patients were all classified in the high-risk group according to the NIH consensus criteria. Two of nineteen patients with stage II had recurrence at the anastomotic site and were treated with imatinib (Gleevec, Norvatis Pharma, Basel, Switzerland). Nine of twelve patients with stage IIIA developed recurrence: 3 patients in the liver, 1 patient in the subphrenic area, 1 patient in perisplenic area, 1 patient in the peritoneum, and 3 patients in the liver with peritoneum. Among them, 1 patient with a solitary liver metastasis underwent radiofrequency ablation and 1 patient with perisplenic metastasis underwent excision. Eight patients received imatinib, but 1 patient recurred before imatinib had been introduced. Eight of sixteen patients with stage IIIB cancer developed recurrence: 4 patients had liver metastasis, 3 patients had peritoneal seeding, and 1 patient had local recurrence in the duodenal stump. All of these patients received imatinib after resection of the recurring tumor or post-ablation.
Table 3.
Descriptive analysis of recurred gastric GIST
|
Variable |
NIH criteria
|
UICC TNM stage
|
|
Stage |
No. |
Stage |
No. |
|
Local recurrence (n = 13)a)
|
Very low |
0 |
I |
0 |
|
Low |
0 |
II |
2 |
|
Intermediate |
0 |
IIIA |
5 |
|
High |
13 |
IIIB |
6 |
|
Peritoneal seeding (n = 6) |
Very low |
0 |
I |
0 |
|
Low |
0 |
II |
0 |
|
Intermediate |
0 |
IIIA |
3 |
|
High |
6 |
IIIB |
3 |
Survival comparison
On univariate analysis, tumor size ≤5 cm (P<0.001), mitotic rate <5/50 HPF (P<0.001), and complete resection (R0) (P<0.001) were favorable predictors of survival. Multivariate analysis showed that a mitotic rate >10/50 HPF (P=0.001), incomplete resection (R1) (P=0.036), and unresectable tumors (R2) (P=0.007) were poor prognostic factors ( Table 4).
Table 4.
Results of multivariate analysis conducted to identify prognostic factors
|
Factor |
Hazard ratio |
95% Confidence interval |
P-value |
|
Resectability |
|
R0 |
1.0 |
- |
- |
|
R1 |
4.4 |
1.097–17.433 |
0.036 |
|
R2 |
4.7 |
1.514–14.399 |
0.007 |
|
Mitotic rate |
|
≤ 10 |
1.0 |
- |
- |
|
> 10 |
11.3 |
2.853–44.726 |
0.001 |
With a median follow-up of 60.1 months (range, 0.4–189.3 months), the overall five-year survival rate was 89.6%. Five-year survival rates were 100% in the very low-, low-, and intermediate-risk groups and 71.9% in the high-risk group according to the NIH consensus criteria (P<0.001). The five-year survival rates according to UICC TNM stage were 100% for stage IA, IB, and II; 75.0% for stage IIIA; 69.5% for stage IIIB; and 55.6% for stage IV (P<0.001) ( Fig. 1). Twelve patients with stage IIIA and fifteen patients with stage IIIB cancers had an over five-year survival rate of 75.0% and 69.5%, respectively (P=1.00). Ten patients had a mitotic rate less than 5/50 HPF but a tumor size greater than 10 cm, which placed them in the high-risk group according to the NIH consensus criteria and classified them as stage II according to the UICC TNM staging system. The five-year survival rate of these 10 patients was 100%. The five-year DFS of the 149 patients who underwent an R0 resection was 86.3%. DFS was also 100% in the very low-, low-, and intermediate-risk groups and 53.1% in the high-risk group (P<0.001). The five-year DFS rates according to UICC TNM stage were 100% for IA and IB, 94.1% for stage II, 41.7% for stage IIIA, 35.1% for stage IIIB, and 50.0% for stage IV (P<0.001) ( Fig. 2).
Fig. 1.
Overall survival (A) by National Institutes of Health consensus criteria (B) and UICC TNM stage (C). 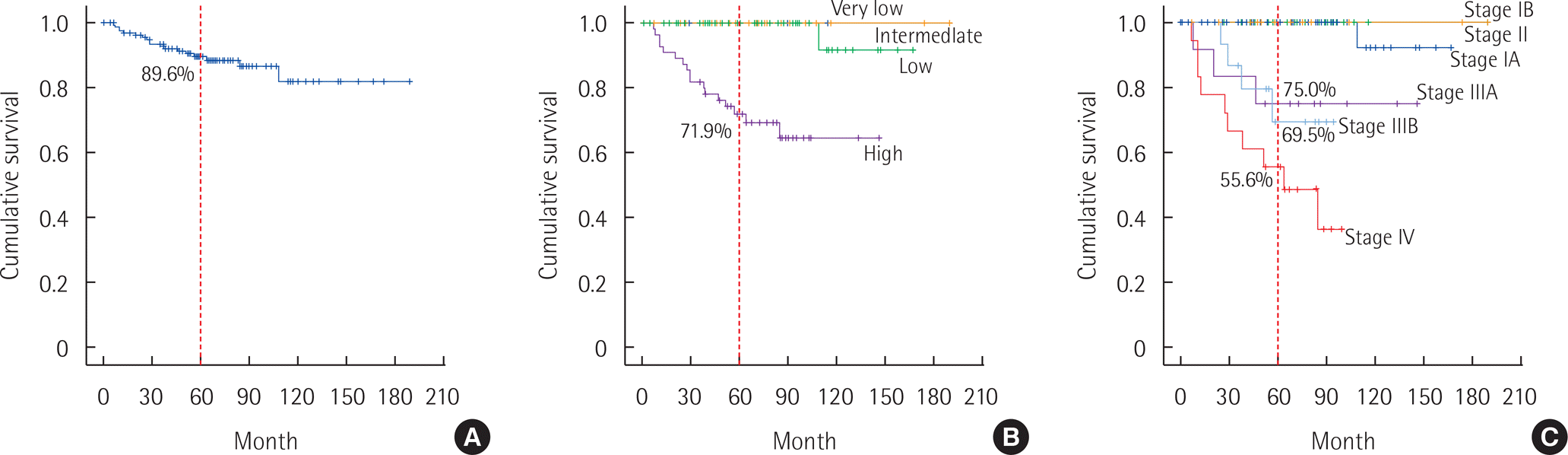
Fig. 2.
Disease-free survival (A) by National Institutes of Health consensus criteria (B) and UICC TNM stage (C) in patients who underwent R0 resection (n=149). 
DISCUSSION
Accurate prognostication of GIST is essential, not only in guiding the clinician with regard to the frequency and intensity of postoperative surveillance but, more importantly, to enable better selection of tumors for potential adjuvant treatment. To date, no study has been conducted to validate the use of the UICC TNM stage versus the NIH consensus criteria or to compare them to determine the optimal risk stratification system for GIST. Here we aimed to provide such a comparison for the first time.
Since the NIH consensus criteria are based on tumor size and mitotic count, this system is easily applied but limited by the biological and prognostic heterogeneity of tumors. For example, patients belonging to the very low-risk groups have an excellent prognosis, but patients belonging to high-risk groups have high recurrence rates and poor prognosis. However, the rate of recurrence and prognosis in patients belonging to the low- and intermediate-risk groups are uncertain [ 15]. Previously published studies from our institution demonstrated that the very low-, low- and intermediate-risk groups have a similar prognosis and prognostic stratification of high-risk GIST is useful for identifying patients with high-risk GIST [ 16, 17]. In this study, the five-year survival rate based on the NIH consensus criteria was near 100% for the very low-, low-, and intermediate-risk groups and 80% in the high-risk group. We were unable to stratify the low- and intermediate-risk groups as was done in the previous reports. Patients with stage IA, IB, and II tumors per the UICC TNM system showed close to 100% survival rates and, therefore, could not be stratified further. Additionally, the five-year survival rates for stage IIIA and IIIB were not significantly different. Patients with stage IIIB cancer had a better five-year survival rate compared to stage IIIA patients. Since the survival rate of stage IIIB patients may have been impacted by the use of imatinib after recurrence, we compared the DFS rates in these patients and found that they were not significantly different (74.1% vs. 76.9%). Therefore, it may not be necessary to stratify stage III into two groups. Our results are consistent with those of a previous study [ 18] that reported the following five-year DFS rates according to AJCC TNM staging: 96% for stage IA, 92% for stage IB, 51% for stage II, 22% for stage IIIA, and 22% for stage IIIB in gastric GIST. The NIH consensus criteria may overestimate the biologic potential for large tumors with a low mitotic rate [ 19]. We found that patients with a low mitotic rate (≤5/50 HPF) and T4 (>10 cm) tumors who were included in the high risk group according to the NIH consensus criteria and were stage II according to the UICC TNM stage had a 100% five-year survival rate. This finding is with that of previously published reports. Until recently, GIST was notorious for being resistant to chemotherapy, with a success rate of less than 5%. Recently, the c-kit tyrosine kinase inhibitor (TKI), imatinib, a drug initially marketed for chronic myelogenous leukemia, was found to be useful in treating GIST, leading to a 40%–70% response rate in metastatic or inoperable cases [ 20– 22]. The two-year survival of patients with advanced disease has risen to 75%–80% following imatinib treatment. However, the optimal duration of adjuvant therapy is currently controversial [ 23– 25]. The multitargeted TKI sunitinib is active in imatinib-refractory or intolerant patients [ 26– 32]. Regorafenib is an orally active TKI that is structurally similar to sorafenib and targets a variety of kinases including KIT, PDGFR, and VEGFRs. Efficacy in refractory patients was shown in a phase II trial of 34 patients who developed resistance to both imatinib and sorafenib, in which four patients had a partial response and 22 had stable disease for 16 weeks or longer; the median PFS was 10 months [ 33]. In conclusion, the result of this study indicates that UICC TNM staging does not appear to be superior to the NIH consensus in the risk stratification of gastric GIST. However, this study includes comparatively small number of patients and future investigation with larger number of sample may demonstrate further prognostic utility. In this study, stage IA, IB, and II patients did not have significant differences in survival. Stage IIIA and IIIB also were not significantly different in terms of survival. However, the high-risk group (T4/low mitotic rate) and stage II appear to be appropriately classified.
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.
REFERENCES
1. Fletcher CD., Berman JJ., Corless C., Gorstein F., Lasota J., Longley BJ, et al. Diagnosis of gastrointestinal stromal tumors: a consensus approach. Hum Pathol 2002;33:459-65.   2. Miettinen M., Lasota J. Gastrointestinal stromal tumors: definition, clinical, histological, immunohistochemical, and molecular genetic features and differential diagnosis. Virchows Arch 2001;438:1-12.   4. Trojani M., Contesso G., Coindre JM., Rouesse J., Bui NB., de Mascarel A, et al. Soft-tissue sarcomas of adults; study of pathological prognostic variables and definition of a histopathological grading system. Int J Cancer 1984;33:37-42.   5. Amin MB., Ma CK., Linden MD., Kubus JJ., Zarbo RJ. Prognostic value of proliferating cell nuclear antigen index in gastric stromal tumors. Correlation with mitotic count and clinical outcome. Am J Clin Pathol 1993;100:428-32.   6. Miettinen M., Makhlouf H., Sobin LH., Lasota J. Gastrointestinal stromal tumors of the jejunum and ileum: a clinicopathologic, immunohistochemical, and molecular genetic study of 906 cases before imatinib with long-term follow-up. Am J Surg Pathol 2006;30:477-89.   7. Miettinen M., Sobin LH., Lasota J. Gastrointestinal stromal tumors of the stomach: a clinicopathologic, immunohistochemical, and molecular genetic study of 1765 cases with long-term follow-up. Am J Surg Pathol 2005;29:52-68.   8. Miettinen M., Lasota J. Gastrointestinal stromal tumors: pathology and prognosis at different sites. Semin Diagn Pathol 2006;23:70-83.   9. Emory TS., Sobin LH., Lukes L., Lee DH., O'Leary TJ. Prognosis of gastrointestinal smooth-muscle (stromal) tumors: dependence on anatomic site. Am J Surg Pathol 1999;23:82-7.   10. Huang HY., Li CF., Huang WW., Hu TH., Lin CN., Uen YH, et al. A modification of NIH consensus criteria to better distinguish the highly lethal subset of primary localized gastrointestinal stromal tumors: a subdivision of the original high-risk group on the basis of outcome. Surgery 2007;141:748-56.   12. Edge SB., Byrd DR., Compton CC., Fritz AG., Greene FL., Trotti A. AJCC Cancer Staging Manual. 7th ed.New York, NY: Springer; 2010.
13. Miettinen M., Majidi M., Lasota J. Pathology and diagnostic criteria of gastrointestinal stromal tumors (GISTs): a review. Eur J Cancer 2002;38(Suppl 5):S39-51.  14. Rudolph P., Chiaravalli AM., Pauser U., Oschlies I., Hillemanns M., Gobbo M, et al. Gastrointestinal mesenchymal tumors – immunophenotypic classification and survival analysis. Virchows Arch 2002;441:238-48.   15. Bucher P., Villiger P., Egger JF., Buhler LH., Morel P. Management of gastrointestinal stromal tumors: from diagnosis to treatment. Swiss Med Wkly 2004;134:145-53.  16. An JY., Choi MG., Noh JH., Sohn TS., Kang WK., Park CK, et al. Gastric GIST: a single institutional retrospective experience with surgical treatment for primary disease. Eur J Surg Oncol 2007;33.  17. Park CK., Lee EJ., Kim M., Lim HY., Choi DI., Noh JH, et al. Prognostic stratification of high-risk gastrointestinal stromal tumors in the era of targeted therapy. Ann Surg 2008;247:1011-8.   18. Rutkowski P., Wozniak A., Debiec-Rychter M., Kakol M., Dziewirski W., Zdzienicki M, et al. Clinical utility of the new american joint committee on cancer staging system for gastrointestinal stromal tumors: current overall survival after primary tumor resection. Cancer 2011;117:4916-24.   19. Miettinen M., Lasota J. Gastrointestinal stromal tumors: review on morphology, molecular pathology, prognosis, and differential diagnosis. Arch Pathol Lab Med 2006;130:1466-78.  20. Heinrich MC., Griffith DJ., Druker BJ., Wait CL., Ott KA., Zigler AJ. Inhibition of c-kit receptor tyrosine kinase activity by STI 571, a selective tyrosine kinase inhibitor. Blood 2000;96:925-32.  21. Tuveson DA., Willis NA., Jacks T., Griffin JD., Singer S., Fletcher CD, et al. STI571 inactivation of the gastrointestinal stromal tumor c-KIT oncoprotein: biological and clinical implications. Oncogene 2001;20:5054-8.   22. Heinrich MC., Blanke CD., Druker BJ., Corless CL. Inhibition of KIT tyrosine kinase activity: a novel molecular approach to the treatment of KIT-positive malignancies. J Clin Oncol 2002;20:1692-703.   23. Verweij J., Casali PG., Zalcberg J., LeCesne A., Reichardt P., Blay JY, et al. Progression-free survival in gastrointestinal stromal tumours with high-dose imatinib: randomised trial. Lancet 2004;364:1127-34.   24. Blanke CD., Rankin C., Demetri GD., Ryan CW., von Mehren M., Benjamin RS, et al. Phase III randomized, intergroup trial assessing imatinib mesylate at two dose levels in patients with unresectable or metastatic gastrointestinal stromal tumors expressing the kit receptor tyrosine kinase: S0033. J Clin Oncol 2008;26:626-32.   26. Debiec-Rychter M., Cools J., Dumez H., Sciot R., Stul M., Mentens N, et al. Mechanisms of resistance to imatinib mesylate in gastrointestinal stromal tumors and activity of the PKC412 inhibitor against imatinib-resistant mutants. Gastroenterology 2005;128:270-9.   27. Demetri GD., van Oosterom AT., Garrett CR., Blackstein ME., Shah MH., Verweij J, et al. Efficacy and safety of sunitinib in patients with advanced gastrointestinal stromal tumour after failure of imatinib: a randomised controlled trial. Lancet 2006;368:1329-38.  
|
|







