INTRODUCTION
Neurofibromatosis type 1 (NF-1, von Recklinghausen disease) is an autosomal dominant hereditary disease and the birth incidence of this disease is 1/2,500 and the prevalence is one in 4,000 live births worldwide [1]. NF-1 was tent to be combined with benign or malignant tumors and multiple gastrointestinal stromal tumors (GISTs) were the most common NF-1-related gastrointestinal tumors.
Multiple GISTs associated with NF-1 were reported in several literatures [2-5] and the incidence was about 7% [6]. Although it was considered to the one type of gastrointestinal involvement in NF-1 (visceral or plexiform neurofibroma), appendiceal neurofibroma in patient with NF-1 was extremely rare, especially with combined multiple small bowel GISTs and this disease was introduced in few literatures in worldwide [7-9]. We present a case of neurofibroma of the appendix and multiple GISTs of small bowel in NF-1 patient.
CASE REPORT
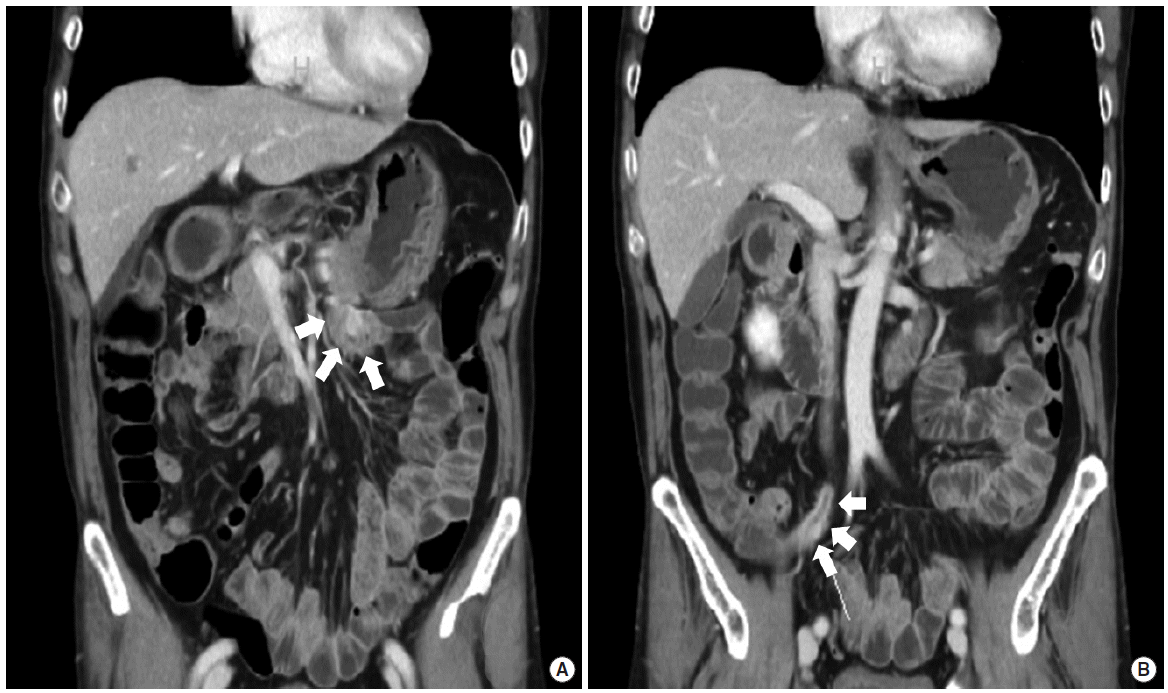
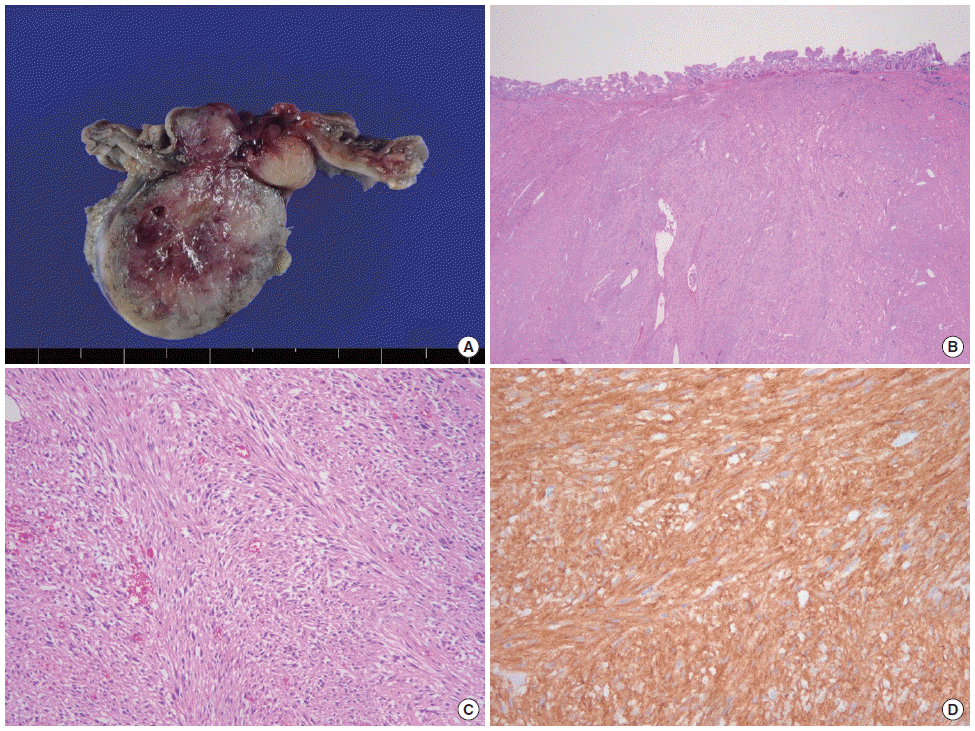
A 61-year-old man was referred to Department of Surgery for operation of appendiceal mass. He had the medical history of hypertension and café-au lait spots and neurofibromatosis on whole skin. The patient’s father and his daughter had also cutaneous neurofibromatosis. Four years ago, he visited our hospital in department of internal medicine with symptoms of epigastric and left upper quadrant abdominal pain. The gastroscopy and abdominal ultrasonography revealed only chronic gastritis and gallbladder polyp. After 1 year from his first visit, he underwent abdominal computed tomography (CT) scan and the CT scan revealed the well-enhancing nodular lesion on proximal jejunum (Fig. 1A). Additional positron emission tomography- CT scan suggested that no fluorodeoxyglucose (FDG) uptakes were observed on any masses on the second portion of duodenum and proximal jejunum. The physician recommended the operation for proximal jejunal masses but the patient refused the operation. Yearly gastroscopy and abdominal CT scan were checked and the last CT scan showed the appendiceal mass which was newly developed after 4 years from his first visit (Fig. 1B). The colonoscopy finding showed the subepithelial tumor on appendiceal orifice and the result of endoscopic biopsy was chronic inflammation (Fig. 2). He decided the operation and he was referred to department of surgery. The patient underwent laparoscopic exploration. The gross finding of appendix in the operative field was nearly normal except the mild thickening of the mid portion of appendix. We performed the laparoscopic partial resection of cecum including appendix using laparoscopic linear stapler for treatment of appendiceal mass. And then we found the multiple (over five) small masses (smaller than 10 mm) on the surface of jejunum and duodenum and one larger mass on proximal jejunum near the Treitz ligament (Fig. 3A). Under the laparoscopic view, dissection of Treitz ligament was performed for mobilization of proximal jejunum and the distal portion of diseased jejunum was transected. We performed the minilaparotomy about 5 cm on upper abdomen just above the Treitz ligament and transected the diseased jejunum near the Treitz ligament. The anastomosis of jejunum was performed via end-to end anastomosis with hand-sewing method (Fig. 3B). One of the multiple small masses on jejunum was resected additionally for diagnosis of these masses. The histological results revealed the appendiceal neurofibroma and two jejunal GISTs. The size of larger jejunal GISTs was 2.7 cm and low mitotic counts (3/50 high power fields) was observed (Fig. 4). And the smaller one (tumor size 0.5 cm) had also low mitotic counts (1/50 high power fields). Two jejunal masses had the positive immunohistochemical staining for C-kit and negative for S-100, desmin and smooth muscle actin. Immunohistochemical staining of appendiceal mass was positive in S-100 protein and very low Ki-67 proliferating activity (Fig. 5). The patient discharged without complication at postoperative day 8 and was alive until now without newly developed mass or other abnormal findings in abdominal cavity.
DISCUSSION
NF-1 is an inherited disease with estimated birth incidence of 1:2, 500–3,000 and autosomal dominant transmission [1].
The major symptoms of NF-1 were cutaneous café-au-lait spots, soft tissue or visceral (plexiform) neurofibromas and additional several types of gastrointestinal and abdominal tumors, including neuronal hyperplasia (neuromas), GISTs, ampullary carcinoid, and pheochromocytoma [10]. Of these combined tumors, GISTs have been reported to be the most common NF-1-assoicated gastrointestinal tumors [2-5,11].
The pathogenesis of GISTs in NF-1 is unclear. Some authors suggested that the lacking KIT or platelet-derived growth factor receptor alpha (PDGRA) mutations were observed in GISTs with NF-1 patients and activation of the Ras-mitogen activated protein kinase signal ing pathway through the somatic inactivation of the NF-1 gene was thought to be the pathogenesis of NF-1-associated GISTs [4,11]. Miettinen et al. [3] analyzed a series of 45 patients with GISTs and NF-1 and suggested that inactivation of the NF-1 tumor suppressor pathway may play an alternative role in GISTs pathogenesis of these patients.
The characteristics of GISTs in NF-1 patients were relatively small with low mitotic activity and are associated with a favorable outcome with no recurrence or metastasis [3,4]. The major involved sites of GISTs are small bowel (53%–68%) and 43%–83% of GISTs were multiple in NF-1 patients [2-4,12]. As mentioned earlier, our NF-1 patient had multiple GISTs that the size was relatively small and located in the jejunum.
On the basis of a single Swedish study of 70 NF-1 patients, it is estimated that adults with NF-1 might have a risk for GISTs as high as 7% [6]. There are a few reports of multiple GISTs with NF-1 in Korea. In one Korean report, 12 patients with multiple GISTs were collected from 50 major university hospitals [4]. Of 12 patients, 5 patients had NF-1 and they had large numbers of small-sized tumor, frequent location in the jejunum, and benign histology. In 2012, Kim et al. [5] reported the oncologic manifestations of NF-1 in Korea and they surveyed NF-1 patients with malignant tumors in Korea. There were 17 GISTs including 3 cases in Kim’s study and the involved site was jejunum. However, it had not been reported to appendiceal neurofibroma and multiple GISTs with NF-1 in Korea and there were few reports in worldwide [7-9,13,14].
Primary tumors of the appendix were rare condition. They were usually diagnosed during pathologic evaluation of the appendix after appendectomy for suspected appendicitis or during the examination of other intraabdominal abnormalities incidentally via abdominal ultrasonography or CT. The benign tumorous condition of appendix consisted of mucocele, tubular adenomas, villous adenomas, leiomyomas, GISTs, lipoma, and neuroma like as our case [15]. In conclusion, our patient had rare condition of appendiceal neurofibroma with multiple jejunal GISTs associated with NF-1. We presented this patient with review of literatures in this article.