Nine months versus 12 months of adjuvant trastuzumab for patients with HER2-positive breast cancer
Article information
Abstract
Purpose
This study aimed to compare the results of treatment with adjuvant trastuzumab for 9 months versus 12 months in human epidermal growth factor 2 (HER2)-positive breast cancer patients. The primary endpoint was disease-free survival. Secondary endpoints included cardiac safety, tolerability, and overall survival.
Methods
The study included 60 non-metastatic HER2-positive breast cancer patients. All study patients underwent surgery, received adjuvant chemotherapy, radiotherapy and hormonal therapy if indicated. Thirty patients were randomized in each group. Group I patients received adjuvant trastuzumab for 12 months, while group II patients received adjuvant trastuzumab for 9 months. Patients were assessed by clinical examination and Echocardiography during treatment.
Results
After median follow-up of 12 months, 90% of the patients in group I were disease free and 83.3% of patients in group II were disease free (P=0.402). All studied population in both groups I and II were alive at the end of the 1-year follow-up period after the completion of adjuvant trastuzumab treatment thus overall survival is 100%.
Conclusion
Trastuzumab is tolerable and its side effects are reversible. Nine months of adjuvant trastuzumab treatment is more cost effective than the standard 12 months.
INTRODUCTION
Breast cancer is considered a major public health problem for women throughout the world. In the United States, breast cancer is still the most frequently diagnosed cancer in women and the 2nd most frequent cause of cancer mortality [1]. Worldwide, breast cancer is the most frequently diagnosed cancer and the leading cause of cancer mortality among females, accounting for 23% of total cancer cases and 14% of cancer deaths, however, there is a 5-fold variation in incidence between high-incidence areas such as the United States and Western Europe, and low incidence areas such as Africa and Asia [1]. In Egypt, breast cancer is estimated to be the most common cancer among females accounting for 37.7% in 2008. It is also the leading cause of cancer related mortality accounting for 29.1% of their total. The incidence to mortality ratio is poor (1.9:1). These estimates are confirmed in many regional Egyptian cancer registries as well as in hospital-based frequencies [2–4].
Women presenting with abnormal imaging findings alone should undergo biopsy guided by mammography (stereotactic biopsy or wire localization breast biopsy), ultrasound, or breast magnetic resonance imaging. Women presenting with a breast mass should undergo fine needle aspiration or core needle biopsy. Newly diagnosed breast cancer cases should be tested for by estrogen receptor (ER) and progesterone receptor (PR) expression and for overexpression of human epidermal growth factor 2 (HER2) receptors [5].
HER2 overexpression accounts for 20% of patients and predicts those who will benefit from HER2-directed therapy. HER2 overexpression is confirmed by uniform intense membrane staining of > 10% of invasive tumor cells (IHC 3+) or the presence of HER2 gene amplification by fluorescence in situ hybridization (FISH) defined as a ratio of HER2/CEP17 (centromeric probe to chromosome 17) ratio ≥ 2.0 [5].
The relationship between HER2/neu protein levels and response to treatment is proportional to the degree of over expression [6,7]. The benefits of adding trastuzumab to adjuvant chemotherapy in patients with HER2-positive tumors was confirmed in a 2012 meta-analysis of eight trials of chemotherapy plus trastuzumab against chemotherapy alone involving nearly 12,000 patients [8]. There was improvement in disease free survival (DFS) regardless of trastuzumab treatment duration or the administration schedule (i.e., concurrent with chemotherapy or sequentially following chemotherapy). The benefit in overall survival (OS) is associated with concurrent administration of trastuzumab with chemotherapy but not with sequential treatment of chemotherapy followed by single agent trastuzumab [9]. The National Comprehensive Cancer Network (NCCN) guidelines recommend a total of 12 months of adjuvant trastuzumab as the standard of care [10] based on the following trials: NSABP B-31, NCCTG N9831 trials, HERA trial, BCIRG 006 trial, PHARE trial. However, there are trials and analysis showing non-inferiority of shorter course of treatment with trastuzumab such as the Short-HER trial and FinHER trial.
METHODS
The present study included female breast cancer patients aged between 18 and 70 years, with histologically confirmed invasive breast cancer, who had HER2-over expression by FISH or silver-enhanced in situ hybridization and had signed informed consent. The study was approved by the Institutional Review Board of Faculty of Medicine, Alexandria University (IRB No. 00007555) and performed in accordance with the principles of the Declaration of Helsinki. Exclusion criteria were: presence of distant metastasis, left ventricular ejection fraction (LVEF) < 50%, pregnancy and having history of thromboembolic manifestations or renal failure.
A total of 60 patients met the inclusion criteria and received adjuvant chemotherapy anthracycline (60 mg/m2), and cyclophosphamide (600 mg/m2) every 21 days for four cycles followed by taxane-based chemotherapy regimen, radiotherapy, hormonal therapy if indicated.
A central randomization procedure was used to assign eligible patients in a 1-to-1 ratio to receive either 12 months or 9 months of trastuzumab. Patients were randomized into two groups: group I included 30 patients who received adjuvant trastuzumab for 12 months that was concurrently administered with taxane-based chemotherapy and group II included 30 patients who received adjuvant trastuzumab for 9 months that was concurrently administered with taxane-based chemotherapy. Trastuzumab was administered by intravenous infusions over 30 to 90 minutes every 3 weeks (initial loading dose 8 mg/kg; 6 mg/kg thereafter) in both groups.
During adjuvant trastuzumab treatment patients were followed up every 3 months by clinical examination and assessment of LVEF by echocardiogram. A decrease of LVEF under 50% or an absolute drop of LVEF of more than 15% from baseline with a LVEF remaining above 50% requires withholding treatment for at least 4 weeks and repetition of assessment of LVEF every 4 weeks then resuming trastuzumab treatment if LVEF returns to normal limits within 4 to 8 weeks and remains at ≤15% decrease from baseline value. Trastuzumab is permanently discontinued for persistent (> 8 weeks) LVEF decline or for > 3 incidents of treatment interruptions.
After the completion of adjuvant trastuzumab treatment patients were followed up every 3 months for 1 year by clinical examination, radiological imaging if needed, assessment of LVEF by echocardiogram and monitoring treatment related side effects.
The primary endpoint was DFS, defined as the time from randomization to the first evidence of recurrence or death or loss of follow-up. Secondary end points included cardiac safety, tolerability, non-inferiority, and OS (defined as the time from randomization and the date of death).
The null hypothesis of the trial was that 9 months of trastuzumab treatment is not inferior to 12 months of trastuzumab treatment by a prespecified acceptable margin in terms of disease survival. The non-inferiority hazard ratio margin of 1.15 was derived from an estimated absolute difference in 1-year DFS of 2%, based on an expected disease survival in the 12-month group of 85% and exponential survival. To conclude non-inferiority (i.e., reject the null hypothesis), the upper bound of the 95% confidence interval resulting from the comparison between the two arms should be less than this prespecified margin. All survival rates for each endpoint were estimated using the Kaplan-Meier method. Hazard ratios were estimated using the semi-parametric Cox proportional hazards model. To evaluate the effect of trastuzumab duration, a Cox proportional hazards model was undertaken on the primary endpoint adjusting for the two variables used for stratification. An interaction test at the 0.10 significance level based on the likelihood ratio statistic for the two-way interaction model was used to test for heterogeneity.
RESULTS
From December 1, 2015 to June 1, 2016, 60 patients were randomly assigned to either 12- or 9-month of treatment with trastuzumab. At the time of the present analysis, median follow-up was 12 months. Patient characteristics were well-balanced between the two groups (Table 1): median age in group I was 45 years while the median age in group II was 46 years. More than half of the patients in both groups were post-menopausal accounting for 56.7% in group I and 60% of patients in group II. More than half of the patients in both groups I and II had pathological tumor size ≤ 2 cm that constituted 50% of patients in group I and 66.7% of patients in group II. Regarding pathological axillary lymph nodes (ALNs) status, most of the patients in both groups had 1–3 (N2) involved ALNs constituting 53.3% of group I patients and 40% of group II. Fifty percent of the patients in group I had lymphovascular invasion compared to 60% of the patients in group II. Thirty percent of the patients in group I had extracapsular extension compared to 50% of group II patients. Regarding Scarff-Bloom-Richardson grade, most of the patients in both groups had grade II disease [11]. Sixty-six point seven percent of the patients in group I and II had ER-positive receptor status. Seventy-six point seven percent of group I patients and 80% of group II patients had PR-positive receptor status. Four patients in group I and three patients in group II (10%) had both ER and PR negative receptor status. Patients in both groups were staged according to the American Joint Committee on Cancer (AJCC) TNM staging system for breast cancer NCCN guidelines version 2.2016. Stage IIA constituted 53.3% of patients in group I and 46.7% of patients in group II, there was no statistically significant difference between both groups when they were compared (P= 0.496).

Comparison between the two studied groups according to age (year), pathological features of the tumor and pathological staging
In this as shown in Table 2 and Fig. 1 the 1-year DFS was 90% in group I and 83.3% in group II there was no statistically significant difference between both groups when they were compared (P=0.402). The 1-year OS was 100% in both groups I and II (no patient died during treatment with trastuzumab or during the study follow up duration).
In group I, as shown in Table 2 and Fig. 1 case relapsed locally at the 12th month of follow-up after the completion of adjuvant trastuzumab treatment. The local relapse was detected by clinical examination in the form of multiple nodules at mastectomy scar, largest 1×1 cm, and confirmed by excisional biopsy. Distant relapse occurred in two patients at the 12th month of follow-up as well. On clinical examination patients had tenderness at right hypochondrium. Aabdomen and pelvis ultrasound was done showing presence of hepatic lesions and the findings were confirmed by abdominal and pelvis computed tomography (CT A/P). None of the patients included in this study required discontinuation of the study due to adverse effect of treatment.
In group II as shown in Table 2 and Fig. 1 local relapse occurred at the 3rd month of follow-up after the completion of adjuvant trastuzumab treatment. Relapse was detected by clinical examination in the form of multiple nodules at mastectomy scar and erythema and confirmed by excisional biopsy. Distant relapse occurred at 6th month of follow-up in one patient who had tenderness over dorsal and lumbar spine on clinical examination and this patient received a bone scan. The bone scan showed multiple bone deposits at DV2-4, LV4, 5 and head of the femur. Also, at the 9th month of follow-up after the completion of adjuvant trastuzumab treatment another patient developed tenderness at the right hypochondrium and had abdominal distension on clinical examination. Abdomen and pelvis ultrasound showed multiple hepatic focal lesions larger than 2× 2 cm and the presence of ascites. The ultrasound findings were confirmed by CT A/P. At the 12th month of follow-up after the completion of adjuvant trastuzumab treatment, one patient had decreased air entry on the left side of the chest on clinical examination. Chest X-ray showed presence of parenchymal lesions and pleural effusion (obliteration of costophrenic angle) and was confirmed by CT chest scan. Another patient had abdominal distension only on clinical examination. Abdomen and pelvis ultrasound was done showing presence of liver deposits. Findings were confirmed by CT A/P.
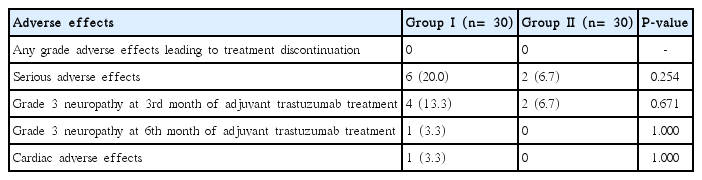
As shown in Table 3 of the patients included in this study required discontinuation of the study due to adverse effect of treatment. Six patients in group I (20%) and two patients in group II (6.7%) developed serious adverse effects during adjuvant treatment with trastuzumab. There was no statistically significant difference when the two groups were compared (P= 0.254). Four patients in group I (13.3%) and two patients in group II (6.7%) developed grade three adverse effects (neuropathy) at the 3rd month of follow-up during adjuvant treatment with taxane-based treatment and trastuzumab. There was no statistically significant difference when the two groups were compared (P=0.671). One patient in group I (3.3%) and no patients in group II (0%) developed grade three adverse effects (neuropathy) at the 6th month of follow-up during adjuvant treatment with trastuzumab. There was no statistically significant difference when the two groups were compared (P= 1.000).
Only one patient in group I (3.3%) developed serious adverse effects in the form of a decrease in the ejection fraction (EF) to 35% at the 6th month of follow-up during adjuvant treatment with trastuzumab, this patient simply required postponing the cycle for two weeks then resuming the treatment as his ejection fraction (EF) recovered to normal values on repeating the echocardiogram (60%) denoting cardiac safety. There was no statistically significant difference when the two groups were compared (P= 1.000).
DISCUSSION
When the DFS of both groups in this study were compared at 1 year, no statistically significant difference was found between the two groups (P=0.402). The DFS for group I was 90.0% and for group II was 83.3%. Proving the non-inferiority of 9 months of adjuvant trastuzumab treatment in comparison to 12 months of adjuvant trastuzumab treatment regarding DFS. Also, the OS of both groups was the same (100%).
In accordance with our results regarding non-inferiority of shorter treatment duration of adjuvant trastuzumab: Persephone, a large phase III randomized noninferiority study was conducted on 4088 HER2-positive early stage breast cancer patients from 152 sites in the United Kingdom and presented during a press briefing in advance of the upcoming 2018 American Society of Clinical Oncology (ASCO) Annual Meeting comparing 6 to 12 months of trastuzumab (Herceptin) in patients with HER2-positive early breast cancer [12].
The 4-year DFS rate was 89% in both arms, the hazard ratio non-inferiority limit was proved (defining non-inferiority as no worse than 3% below the 12-month arm). Congruent results were found for OS. Cardiac events were reduced in patients on the 6-month arm (4%, compared with 8% of patients on the 12-month arm stopping treatment due to cardiotoxicity, P< 0.0001) [12].
Multiple studies had been conducted that compared 9 weeks of adjuvant trastuzumab versus standard 52 weeks: Conte et al. [13] in the Short-HER study, included HER2-positive patients with either node positive or high-risk node negative having mean age of 55 years. Patients were randomized to receive either the shorter treatment, including three courses of docetaxel given every 3 weeks plus trastuzumab given weekly for 9 doses, followed by three courses of 5-fluorouracil/epirubicin/cyclophosphamide, or standard 12-month treatment with four courses of anthracycline-based chemotherapy followed by four courses of docetaxel in combination with trastuzumab given every 3 weeks, followed by 14 additional courses of trastuzumab given every 3 weeks (for a total of 18 doses). Radiation therapy was administered when indicated after chemotherapy, and hormonal therapy was started after completion of chemotherapy in patients with hormone receptor-positive tumors. He reported at the annual meeting of the ASCO on 2017 that 9 weeks of treatment with trastuzumab resulted in comparable DFS and OS to that seen with the standard 12 months of trastuzumab, with about one-third of the rate of severe cardiac toxicity in patients with HER2-positive early breast cancer.
The 5-year DFS rate in 626 patients who received 9 weeks of trastuzumab was 87.5%, compared with 85.4% in 627 patients who received 1 year of trastuzumab therapy. The secondary endpoint of OS was also similar in the two groups (95.1% vs. 95.0%; hazard ratio= 1.06).
The SOLD trial that was presented at San Antonio in 2017 by Joensuu et al. [14] who studied whether it is sufficient to administer trastuzumab with chemotherapy only for a brief period of time (9 weeks) instead of the standard practice of administering trastuzumab both during chemotherapy (for 9 weeks) and then as a single agent after stopping chemotherapy (for total of 12 months). Patients in the 9-week arm received no further treatment, whereas those in the 12-month arm received trastuzumab every 3 weeks for 14 cycles. Patients with ER-positive cancer received appropriate endocrine treatment and radiation therapy per the guidelines. In the 12-month arm, the DFS rate was 90.5%, compared with 88% in the 9-week arm. There was no difference in distant DFS and OS between the two arms: 5-year distant DFS was 93.2% in the 9-week arm and 94.2% in the 12-month arm; 5-year OS was 94.7% in the 9-week arm and 95.9% in the 12-month arm.
Sendur et al. [15] in 2014 retrospectively analyzed patients with HER2-positive, node-positive breast cancer who received adjuvant Herceptin for 9 weeks and 52 weeks. With a median follow-up of 34 months, there was no difference in DFS (P= 0.76) and OS (P= 0.99) at years 1, 3, and 5. Asymptomatic decline of LVEF was observed in 1.9% and 15.5% of patients in the 9-week and 52-week treatment groups, respectively (P<0.001). Tonyali et al. [16] in 2012 compared results of 479 consecutive women who received adjuvant Herceptin for 9 weeks or 52 weeks at eight centers. The median duration of follow-up was 30 months. Results at 36 months for DFS and OS were similar in the two groups. The DFS rate was 90% vs. 85% for 9 weeks vs. 52 weeks respectively (P= 0.132) and the OS rate was 96% vs. 97% respectively (P=0.779). Recurrences were observed in 8.3% vs. 11.7% and death occurred in 2.7% and 2% of patients treated for 9 weeks vs. 52 weeks, respectively. No deaths were considered related to Herceptin. In the 9-week group, one patient each experienced asymptomatic EF decline, symptomatic EF decline, and grade 3 allergic reaction. In the 52-week group, adverse events were asymptomatic EF declines in eight patients, symptomatic EF declines in four patients, and grade 3 allergic reaction in one patient. Icli et al. [17] in 2011 conducted a retrospective study comparing DFS in patients who received adjuvant Herceptin for 9 weeks vs. > 9 weeks and reviewed the Turkish Ministry of Health records of 690 HER2-positive breast cancer patients. Median follow-up duration was 22 months. At 2 years, DFS in patients who received Herceptin for 9 weeks was 85.6% compared with 85.4% in patients who received Herceptin for > 9 weeks (P=0.28). Cardiac toxicity leading to interruption of Herceptin therapy was reported in 0% of patients in the 9-week group and 3.3% of patients in the > 9-week group. Ozen et al. [18] in 2010 retrospectively studied the use of 9 weeks of Herceptin administered either concomitantly with or after adjuvant chemotherapy in 102 women with HER2-positive breast cancer. Only one local recurrence and no distant metastases were observed at a median follow-up of 1 year.
On the contrary, others recommended adjuvant treatment with trastuzumab for 12 months: Pivot et al. [10] in 2013 in the PHARE trial which is an open-label, randomized, phase 3 trial in 156 centers in France randomly assigned 1,691 patients to receive 12 months of trastuzumab and 1,693 to receive 6 months of trastuzumab. He found after a median follow-up of 42.5 months, 175 DFS events in the 12-month group and 219 in the 6-month group. Two-year DFS was 93.8% (95% confidence interval [CI], 92.6–94.9) in the 12-month group and 91.1% (95% CI, 89.7–92.4) in the 6-month group (P= 0.29). After 3.5 years of follow-up, Pivot et al. [10] failed to show that 6 months of treatment with trastuzumab was non-inferior to 12 months of adjuvant trastuzumab. Thus, it was determined that 12 months of adjuvant treatment with trastuzumab should remain the standard of care.
Goldhirsch et al. [19] in 2013 at the HERA trial reported after an 8-year median follow-up period, statistically significant improvements in DFS with Herceptin for 1 year compared with observation (P< 0.0001). OS was also statistically significantly improved for patients treated with Herceptin for 1 year compared with chemotherapy alone (P= 0.0005). The final analysis of HERA also compared DFS in patients treated with Herceptin for 2 years to 1 year. Results showed that DFS for patients who received Herceptin for 2 years compared with 1 year was not statistically significantly different (75.8% vs. 76%, P= 0.86). OS in patients treated with Herceptin for 2 years compared with 1 year was also not statistically significantly different. Also, Romond et al. [20] in December 2012, in a San Antonio Breast Cancer Symposium reported the findings of the joint analysis of NSABP B-31 and NCCTG N9831 Trials. For the Herceptin treatment arm, the DFS rate was 73.7% compared with 62.6% for the chemotherapy alone arm, with a 40% reduction in the risk of a DFS event in the Herceptin treated group (P< 0.0001). OS was also statistically significantly improved for Herceptin-treated patients compared with patients treated with chemotherapy alone and resulted in a 37% reduction in the risk of death.
Of note no study was conducted beforehand that compared 9 months of adjuvant trastuzumab treatment to the standard 12 months.
It is important to consider that this study included only 60 patients who were followed up for 1 year. Only 60 patients were included due to the cost of HER2 testing and trastuzumab is quite an expensive drug making its affordability quite difficult. The 1-year follow-up duration was set as we were restricted to a due date to finish the study and defend the thesis the study is part of.
The results of the present study showed that only one patient in group I (12 months group) EF dropped during the 6th month of treatment from 64% to 35%. For this patient the trastuzumab was just delayed for 2 weeks after which the patient EF was recovered > 50%. No patient in group II had any cardiac toxicity.
Joensuu et al. [21], reported one case of symptomatic heart failure from 2 to 35 months after study entry in one Herceptin-treated patient and two patients who received chemotherapy alone. While median LVEF decreased from baseline in the comparison group (66%–62%, P= 0.006), median LVEF (65%) in patients treated with Herceptin did not change during follow-up [21,22].
Several studies found that exposure to anthracyclines, low baseline EF, older age, hypertension and high body mass index appear to predict a higher likelihood of cardiac toxicity. This explains the low incidence of cardiac toxicity in our study as the median patient age in group I was 45 years and 46 years in group II. All patients included in our study had normal base line EF ( >50%) in both groups. Only three patients in group I and three patients in group II had hypertension [23–25].
Several studies have reported genetic alterations within the HER2 receptor that may predispose to cardiac toxicity from trastuzumab due to single nucleotide polymorphisms (SNPs) that have been associated with enhanced drug efficacy and toxicity in cancer therapy. SNP variations in the ErbB2 gene have been identified that alter the protein sequence of the HER2-neu protein. Only two of the ErbB2 SNPs (Ile 655 Val and Pro 1170 Ala) were found to have variation. The HER2/neu Pro 1170 Ala polymorphism can be used to identify a subset of patients who are at increased risk of cardiotoxicity from trastuzumab therapy [26–28].
However, Pivot et al. [10] reported a significantly higher rate of congestive heart failure (CHF) for those receiving 1 year of therapy compared with 6 months in the PHARE study, but the rates were very low in both arms with recovery in the vast majority of patients. Schneider et al. [29] found that one out of 234 patients (3%) had CHF including one patient with grade 3 myocarditis; three of the patients were on the abbreviated arm and four on the conventional arm. There were no differences between Arms in the proportion with LVEF decrease >10% post-docitaxol-herceptin treatment (P= 0.6) or post-adryamicin-cyclophosphamide therapy (P= 0.6). Compared with 12-week treatment with trastuzumab, 1 year of trastuzumab-based therapy did not increase the frequency or severity of cardiac toxicity: three patients on the abbreviated Arm and four on the conventional Arm experienced CHF. In our study regarding the tolerability of patients to treatment in both groups, findings detected on clinical examination during adjuvant trastuzumab treatment were not different between the two groups, were resolved after completion of adjuvant trastuzumab treatment and were tolerable.
From the results of this study regarding the absence of statistically significant difference in DFS and OS between the 12- and 9-month groups together with having Egypt a developing low-tomiddle income country. We can suggest that 9 months of adjuvant trastuzumab treatment is non-inferior to 12 months of adjuvant treatment regarding the DFS and OS. That shorter duration of adjuvant trastuzumab treatment is less cardiotoxic and more tolerable than a longer one. A large multicenter trial needs to be conducted that should include a larger number of patients to be followed up for longer durations, leading to strong evidence that can change the guidelines.
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.