INTRODUCTION
Incidental ingestion of a foreign body is common in children and psychiatric patients. In most cases, ingested foreign bodies pass through the gastrointestinal tract without complications [1]. Ingested foreign bodies may result in complications such as perforation, hemorrhage, or fistula [2]. Intestinal obstruction following ingestion of a foreign body is a complication which needs surgical treatment.
Generally, patients with clinical features of intestinal obstruction without a history of prior laparotomy or physical evidence of a hernia could be a diagnostic challenge. The most common cause, however, of colonic obstruction in these patients is malignancy.
In adults, intestinal obstruction after ingestion of a foreign body is a not uncommon condition which is reported more frequently in elderly because of their dentures. Therefore incidental diagnosis or preoperative detection of malignancy in these patients is critical for optimal treatment planning.
An incidental finding of colon cancer is uncommon. Screening colonoscopy or other diagnostic tools can help to find undiagnosed colon cancers [3,4]. Incidental discoveries of colon cancer, however, in the work-up or treatment of other medical conditions are rare. There have been only a few case reports of incidentally detected colon cancers in the literature [5,6].
We report a case of the incidental diagnosis of an ascending colon cancer after intestinal obstruction due to ingestion of beef bones.
CASE REPORT
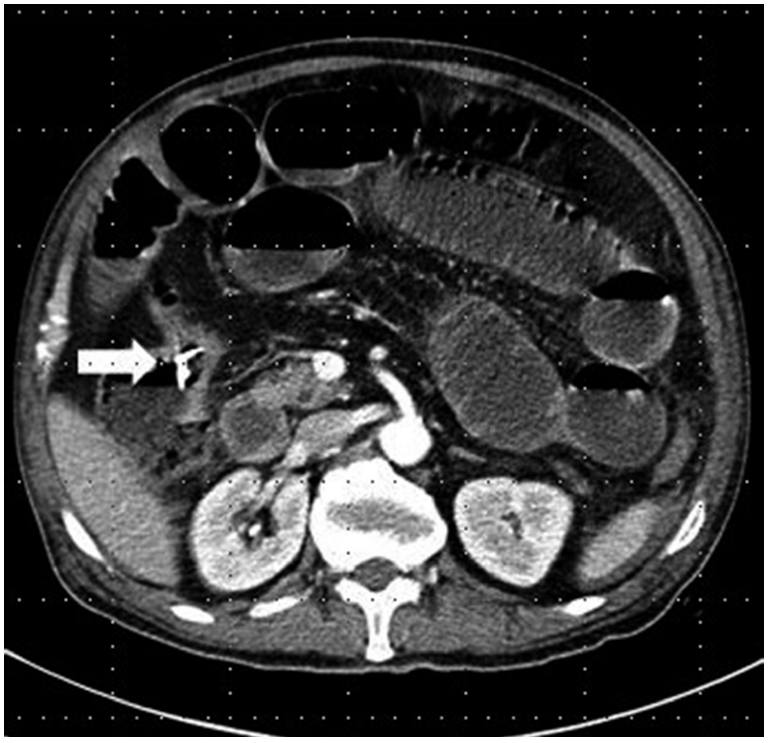
A 75-year-old man visited the emergency room with abdominal distension and intermittent vomiting for 5 days. Vital signs were stable. On physical examination, the abdomen was soft but distended without tenderness. Plain abdominal radiograph showed distended loops of the small intestine and a small foreign body in the ascending colon (Fig. 1). The patient had a history of taking Korean beef bone soup seven days ago. An abdominal computed tomography (CT) scan revealed an ascending colon cancer with an impacted foreign body that was causing intestinal obstruction (Fig. 2). The hemoglobin level was 4.6 g/dL. The patient transfused with six packed red blood cell prior to the surgery.
The intestinal obstruction was treated with conservative management including nasogastric decompression, nil per os and intravenous hydration. After two days, the intestinal obstruction resolved and the nasogastric tube was removed.
On the fifth day after admission, colonoscopy showed an encircling mass causing luminal narrowing in the ascending colon (Fig. 3. The scope could not be passed beyond the mass. Biopsies of the colon mass tissue were taken during the colonoscopy. Histology revealed adenocarcinoma of the colon.
Positron emission tomography-CT scan showed no signs of distant metastasis.
Elective surgery for the ascending colon cancer was delayed because of preoperative evaluation. On the 11th day after admission, laparoscopic assisted right hemicolectomy was performed. It was, however, converted to an open procedure because of the large size of the tumor and severe adhesions to adjacent tissues. The small intestine, cecum, and ascending colon were dilated and edematous in spite of conservative treatment with nasogastric decompression and nil per os. Ischemia or perforation of the intestine proximal to the obstructing colon cancer was not shown. Ileocolic anastomosis was performed with double stapling method using linear staplers. Interrupted 3-0 silk sutures were placed using an inverting Lembert stitch around the anastomosis. The security of the anastomosis was confirmed and a diverting loop ileostomy was not created.
Two bone-like materials were shown in the ascending colon when the specimen was opened in the operating room. They measured 1.7×1.1 cm and 2.2×0.6 cm and were pathologically confirmed as cortical bone fragments (Fig. 4). Pathologically, the ascending colon cancer with a size of 5.6×6.3 cm was a moderately differentiated adenocarcinoma with invasion through the muscularis propria into pericolic tissues and there was no regional lymph node metastasis (pT3N0M0).
At postoperative day 2, the patient had a fever (38.3°C). A small amount of bile-stained fluid was drained via a closed suction drain placed in the right paracolic gutter from the fifth postoperative day. The patient had a complaint of mild abdominal pain. Broad-spectrum antibiotics were used to treat the intra-abdominal infection.
At postoperative day 8, the amount of drainage was increased and abdominal pain became progressively worse. Exploratory laparotomy was done and anastomotic leakage was detected. Staple line disruption occurred at the distal end of the longitudinal staple line between the ileum and colon and the point at which longitudinal and transverse staple lines crossed. Primary closure of the anastomosis and a diverting ileostomy were performed.
Acute kidney injury induced by the long-term use of intravenous antibiotics including vancomycin occurred during the postoperative period. It resolved after transient hemodialysis treatment.
Deep surgical site infection was developed after the second surgery and partial abdominal wound dehiscence occurred. On the 33rd day after the primary surgery, the patient underwent repair of wound dehiscence.
The patient was discharged on the 42nd day after the primary surgery with a completely healed incisional wound and normal kidney function.
DISCUSSION
More than 80% of ingested foreign bodies pass without the need for intervention [7]. However, ingested foreign bodies may result in bowel obstruction, perforation, ulcer, laceration, hemorrhage, abscess, fistula, and bacteremia [2]. Foreign body impaction, bowel perforation or obstruction commonly occurs at the site of acute angulation or narrowing. Patients with prior gastrointestinal tract surgery or congenital gut malformations are at increased risk for obstruction or perforation [8]. The patient of this case had no history of previous abdominal surgery and been well without abdominal pain requiring surgical intervention. The beef bone was lodged in the colon cancer which had not been detected before the intestinal obstruction had developed.
In the literature, ingested bones included usually fish bones and chicken or poultry bones, not beef bones [2,5,6]. In this case, the patient ingested beef bones.
The incidental finding of colon cancer following the ingestion of foreign bodies is uncommon. In the literature, there have been not many reports about colon cancer diagnosed after the ingestion of a foreign body. Some authors have reported colon cancers discovered after bowel perforation caused by ingested foreign bodies [5,6]. Few cases of colon cancer diagnosed by colon obstruction following ingestion of a foreign body have been reported [9].
Intestinal obstruction caused by the impaction of a foreign body may occur more frequently in patients who have advanced-stage colon cancer. In the patient with advanced-stage colon cancer, the size of the colon cancer may be large enough to impede the passage of the foreign body. Obstruction can, however, even be possible in patients with early-stage colon cancer. The large foreign body might become stuck in an early colon cancer which is small but located at an angulated or narrow site in the colon. In this case, the colon cancer was large (5.6×6.3 cm) and was stage IIA (pT3N0M0).
Colon cancer is thought as the initial cause of intestinal obstruction in this case. As the colon cancer had grown, the lumen had become narrow. The patient had not recognized the symptoms of the colon cancer until the obstruction occurred. When the ingested beef bones could not pass through the narrow colon lumen, the colon obstruction developed. It would be thought that if the large foreign body was ingested in early stage colon cancer, the colon cancer could be diagnosed earlier. The large foreign body, however, may lodge in the proximal gastrointestinal tract having narrower lumen than the colon and the colon cancer could not be diagnosed.
In previous case reports, foreign body-associated bowel obstruction or perforation with previously undiagnosed colon cancer commonly occurred at the point of acute angulation and in the sigmoid colon with narrow lumen [5,6]. In present case, bowel obstruction by ingested foreign bodies occurred in the ascending colon with relatively large caliber. It seems to be caused by the wedge shape of the ingested beef bone lodging easily at the colon wall and by colon lumen narrowing due to the large size of the ascending colon cancer.
Elderly patients have a greater tendency to unintentionally swallow foreign bodies compared to younger patients. They have decreased oropharyngeal function to remove foreign bodies and they also have poorer dentition. These factors make it harder for elderly patients to eliminate foreign bodies that have been accidentally ingested.
CT scan is a good modality for the accurate detection, characterization, and determination of the clinical significance of ingested foreign bodies [10]. Although the foreign body was detected in a plain abdominal radiograph in this case, the CT scan offered more information about its location and relationship with the colon cancer. CT scan images also provide information about the presence or absence of colon perforation, pericolic abscess, or hemorrhage.
There are many risk factors for anastomosis leakage including malnutrition, weight loss, alcohol intake, long operation time, intraoperative contamination, and blood transfusions [11]. In present case, the patient had risk factors; poor nutrition status due to delayed surgery, and preoperative blood transfusions. Edema of the small bowel wall resulting from intestinal obstruction, also, could be a major predisposing risk factor for anastomosis leakage in this case.
Colon obstruction following ingestion of foreign body in elderly patients, especially without a history of laparotomy, may be a sign of colon cancer. Surgeons should be aware that colorectal cancer could be a cause of intestinal obstruction when the patient has a history of ingesting a foreign body and the foreign body lodges in the colon and rectum.